By Saloni Nagar, Medically Reviewed by Dr. Jimisha Shah, B.V.Sc & A.H., PGDAW
Cats should not go more than 24 hours without food, and even within the first 12 to 24 hours, their bodies begin a chain of internal changes that place real strain on the liver, the brain, and the systems that manage metabolic waste.
Understanding how long a cat can survive without food is not abstract biology; it is one of the most practically important things a cat owner can know.
This is also one of the most widely misunderstood areas of cat care. Many loving owners assume that cat appetite loss only becomes worth worrying about after several days of food refusal. A cat turning its nose up at a meal can look like pickiness, a passing mood, or a minor preference change. In some cases, it genuinely is.
But the biology underneath tells a more complicated story, one where the window between “my cat seems a little off” and “this needs veterinary attention” is shorter than most people expect.
Unlike humans or dogs, cats have no meaningful ability to slow their metabolism or adapt their energy systems when food disappears. Their bodies are calibrated for continuous protein intake, and when that intake stops, the internal response is not a gentle conservation mode.
It is an active, ongoing process that produces waste products the body must manage, and that management depends on nutrients that are only available through food.
This article explains what happens during the first 24 hours of a cat not eating, which cats face the greatest risk of rapid decline, and how symptoms can escalate from subtle behavioral shifts to something more serious faster than most owners anticipate. Understanding these patterns early is one of the most meaningful things a caring pet parent can do.
Metabolic Consequences of Missed Meals in Cats
The danger of cats not eating is not always obvious from the outside. A cat sitting quietly near a window, uninterested in its bowl, may look peaceful rather than unwell. But the biology beneath that stillness tells a different story, one rooted in how feline metabolism actually works and why cats cannot skip meals the way other animals sometimes can.
Cats are obligate carnivores a biological classification that shapes everything about how their bodies process energy, protein, and waste. This is not a dietary preference. It is a metabolic reality that makes even a single day without food genuinely consequential in ways that do not apply to dogs or humans.
if you want to know more about why cats are obligate carnivores read our detailed article on –Why Cats Lose Muscle but Gain Fat: An Obligate Carnivore’s Guide to Protein (2026)
According to the Cornell University College of Veterinary Medicine, anorexia can have a severe impact on a mature cat’s health if it persists for as little as 24 hours. That figure comes from institutional veterinary guidance not from worst case speculation. It reflects how quickly feline metabolism responds when nutrients are withdrawn.
The sections below examine three distinct questions that build on each other: what the body is actually doing during those first 24 hours, whether a single skipped day constitutes real risk, and how to tell the difference between a cat being picky and a cat showing early signs of metabolic strain.
What happens if a cat doesn’t eat for 24 hours?
Within 24 hours of not eating, a cat’s body depletes its available glucose and shifts into a protein based energy state, a transition that begins generating metabolic waste and placing early strain on the systems responsible for clearing it. This internal shift begins within hours of the last meal, not days, and its visible expression is the subtle behavioral quietness many owners notice but do not immediately connect to food refusal.
In a fed cat, energy comes primarily from dietary protein. When food is no longer available, blood glucose drops and the body moves to its next available resource. In cats, this transition leads rapidly to protein catabolism the breakdown of amino acids, including from muscle tissue, to sustain essential functions.
This process produces nitrogen as a byproduct, which converts to ammonia and enters the bloodstream. The liver must then process and clear that ammonia a task that depends on a continuous supply of specific amino acids, most critically arginine. The deeper explanation of how that dependency works, and what happens when it is disrupted, is covered later in this article.
What matters at this stage is understanding that the sequence begins within the first day and that the behavioral signals owners may notice, such as reduced activity and a quieter, more withdrawn quality, are the visible surface of an internal process already underway.
Cats don’t “handle fasting” like humans or even dogs.
Their metabolism is wired to expect frequent protein intake, and even short food gaps can trigger fat mobilization in the liver a dangerous process that can escalate silently.This tool doesn’t just track time.
It helps you interpret risk based on physiology, not guesswork.
🐱 Cat Fasting Risk Calculator
Advanced risk analysis using time, age, weight, and symptoms.
Is it dangerous if my cat skips meals for a day?
Skipping food for a full day is not safe for cats. Unlike dogs or humans, cats have no way to reduce their rate of protein consumption during food scarcity.
Internal processes produce and must clear metabolic waste at a similar rate, even if no food is provided. This metabolic inflexibility makes a day without food much riskier for cats than for most other domestic animals.
Dogs have some capacity to accommodate a short fast; their metabolic pathways allow a degree of flexibility. Humans can adapt considerably further, entering alternative energy states that sustain function for extended periods. Cats have none of this flexibility, essentially.
Research from the Ontario Veterinary College (Verbrugghe and Bakovic, 2013, Nutrients, PMC) documents this clearly: cats maintain a consistently high rate of protein oxidation and are unable to adapt to reduced protein intake, a fact that distinguishes them from virtually every other common domestic animal.
The risk is significantly amplified when the cat is already unwell, elderly, or falls into one of the higher vulnerability groups discussed later in this article.
A healthy adult cat that has missed one meal and is otherwise behaving completely normally is in a different position from a cat that has gone a full day without eating and is also showing behavioral changes.
Both situations warrant attention, but the second warrants it more urgently.
If your cat stops eating, what you do in the next few hours matters more than anything else.
This quick action guide gives you exactly what to do—step by step—without overthinking
- 24+ hours without food
- Any symptoms appear
- Your cat is overweight or already sick
Can a cat skip meals and still be healthy?
Weakness, alongside meal skipping, is not normal feline behavior; it is an early signal that the body's energy systems are already under strain, and it reflects a genuine internal change rather than a passing mood. While occasional appetite variation exists in healthy cats, a cat that is both refusing food and visibly less energetic than usual is showing two signals at once that together carry more weight than either would alone.
Cats are natural small-meal eaters. In their natural state, they hunt and consume multiple small portions throughout the day, and their appetite consistency under domestic conditions is one of the more reliable indicators of their overall health. Veterinarians commonly use changes in appetite as an early assessment marker precisely because they tend to accurately reflect systemic status.
What weakness, alongside food refusal, often indicates is that the body has already begun drawing on internal resources and that the physical fatigue is a direct expression of that process. It is easy to attribute this to a cat simply having a tired day, and many caring owners do exactly that.
There is an important distinction between a cat that occasionally eats less at one meal and a cat that has genuinely stopped eating. If your cat’s behavior is also visibly shifting alongside food refusal, do not wait—contact your veterinarian promptly for advice and evaluation..
Not every behavior change is dangerous but some are early warning signs you shouldn’t ignore.
This table helps you quickly tell the difference between normal variation and potentially serious symptoms, so you can respond with confidence.
| Normal Behavior (Monitor) | Concerning Behavior (Act Now) | What It Likely Means | What You Should Do |
|---|---|---|---|
| Slight drop in appetite (still eating a little) | Complete refusal to eat | Appetite regulation vs metabolic shutdown | Monitor closely; if no improvement in 12–24 hrs, escalate |
| Mild tiredness or sleeping more | Weakness, difficulty standing, or unsteady movement | Energy conservation vs systemic stress | Encourage food; seek vet advice if worsening |
| Eating slower than usual | Sniffing food but refusing to eat | Possible nausea or early illness | Try different food; monitor for additional symptoms |
| Less playful but still responsive | Hiding, avoiding interaction, isolating | Behavioral change due to discomfort or pain | Check environment; treat as early warning sign |
| Occasional skipped meal | No food intake for 24+ hours | High risk of metabolic complications | Immediate veterinary consultation |
| Normal drinking habits | Reduced water intake or dehydration signs | Fluid imbalance or illness progression | Encourage hydration; monitor closely |
| Normal grooming | Neglecting grooming, messy coat | Low energy or declining health | Observe closely; combine with other symptoms |
| Calm behavior | Irritability, unusual aggression, or extreme quietness | Stress, pain, or neurological involvement | Do not ignore—watch for escalation |
| Alert and aware | Confusion, disorientation, or staring | Neurological impact (serious stage) | Urgent veterinary attention needed |
| No physical symptoms | Vomiting, drooling, or yellowing (eyes/gums) | Toxic buildup or liver stress | Emergency care required |
Feline Metabolism and Why Cats Cannot Go Without Food
One of the most persistent misconceptions in everyday cat care is that cats are naturally self-regulating eaters who can skip meals occasionally without meaningful consequence.
This belief often comes from a genuine experience of an owner who has seen their cat refuse a meal, waited it out, and watched the cat eventually eat again without obvious harm. That experience is real. But it does not reflect what was happening inside the cat's body during that interval.
The myth that cats can fast without harm is particularly persistent because cats often do not show dramatic visible distress in the early stages of food deprivation.
They may rest more, move less, or withdraw slightly, signals that are easy to read as mood rather than metabolic strain. Without obvious symptoms, the situation can look benign when it is not.
Understanding why this myth is genuinely dangerous requires looking at feline biology directly.
This section builds that picture across four distinct layers: what makes cats biologically different from other animals when it comes to fasting, what their daily protein requirements actually involve, the full internal sequence of what happens when food is skipped, and the specific vulnerability that sits at the center of feline food deprivation risk.
Why can’t cats fast like dogs or other animals?
Cats cannot fast safely because their metabolism is permanently set to process protein at a high rate, regardless of food availability, and unlike dogs or humans, they have no enzymatic pathway to reduce this consumption or switch efficiently to alternative fuel sources when food is absent. This is not a matter of degree but of fundamental metabolic architecture.
The classification of cats as obligate carnivores carries specific and measurable physiological weight. It means that the enzymatic systems governing energy production in cats are built around the assumption that animal-source nutrients will always be present. The fasting adaptation mechanisms that exist in other species, such as reducing the rate of protein catabolism, shifting to ketone-based energy production, or entering a metabolic conservation state, are either absent or severely limited in cats.
Research from the Ontario Veterinary College, Verbrugghe and Bakovic, 2013, Nutrients, PMC documents this directly: cats have a consistently high rate of gluconeogenesis and protein oxidation that does not downregulate during food restriction. This is what makes the continuous protein need in cats a metabolic requirement built into their physiology rather than simply a dietary guideline.
When food disappears, the metabolic engine does not slow; it continues running, drawing on whatever protein is available.
Complex explanations can be confusing—but the core idea is actually simple.
This quick breakdown gives you the one truth that explains everything happening inside your cat’s body.
When they stop eating, their body doesn’t switch safely to fat—instead, it begins breaking down its own protein stores.
This process produces toxic byproducts like ammonia, which can affect the brain and nervous system rapidly.
Why do cats need protein every single day?
Cats require a daily supply of specific essential amino acids, including arginine, taurine, and methionine, because their bodies use these compounds at a high rate and cannot synthesize or conserve them in quantities sufficient to bridge even a short dietary gap. This daily dependency is what makes food refusal metabolically consequential so quickly.
The amino acids cats require go considerably beyond what most owners might assume from the label on a bag of cat food. Arginine, taurine, methionine, and cysteine are all essential for cats in quantities greater than those required by dogs or most other species. According to research published in Nutrients, Verbrugghe and Bakovic, 2013, PMC, cats have a hastened rate of use of these amino acids combined with an inability to conserve them, making higher and continuous dietary intake a functional necessity.
These amino acids serve roles across the entire body. Taurine supports heart function and vision. Methionine contributes to liver health and protein synthesis. Arginine, which will be examined in detail in the next section, is the linchpin of the process that clears ammonia from the blood.
When the daily intake of these compounds is interrupted, the body does not place these processes on hold. It begins sourcing what it needs from muscle tissue, accelerating physical deterioration while simultaneously increasing the metabolic waste load the body must manage.
A cat that has been well nourished has a small buffer of these amino acids in circulation. But research from the Ontario Veterinary College confirms that even in naturally developing cases of food deprivation, these buffers deplete meaningfully, with plasma concentrations of arginine, taurine, and methionine falling by more than 50% in cats with hepatic lipidosis Verbrugghe and Bakovic, 2013.
Many cat owners believe that skipping meals simply leads to hunger.
But inside your cat’s body, something far more dangerous happens. This visual breaks down the “protein → energy” pathway vs. the “protein breakdown → toxin” trap—so you can see exactly why even short fasting periods can become life-threatening.
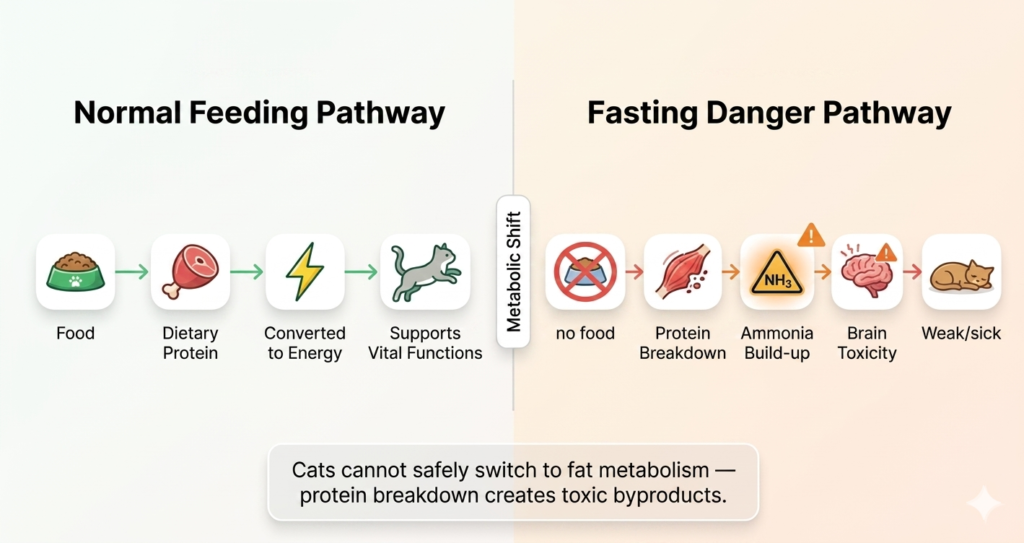
What happens inside a cat’s body when it skips food?
When a cat stops eating, the body enters a catabolic state in which muscle tissue is broken down for energy. This raises the liver's workload, depletes the amino acids needed to manage metabolic waste, and creates a compounding internal strain that intensifies the longer food is withheld. This is not a gradual or gentle process in cats; it is an active metabolic shift with measurable physiological consequences.
Building on the earlier overview of the first 24 hours, the fuller picture of what happens inside a fasting cat involves three compounding processes occurring simultaneously. First, protein catabolism accelerates as the body sources amino acids from muscle for gluconeogenesis. Second, this breakdown produces increasing amounts of nitrogen waste, which converts to ammonia in the gut and is absorbed into the bloodstream. Third, the liver, already receiving a rising load of fatty acids from fat stores being mobilized for energy, must simultaneously manage the growing ammonia load.
Research from the Ontario Veterinary College, Verbrugghe and Bakovic, 2013, confirms that in cats experiencing hepatic lipidosis from food deprivation, multiple critical amino acids fall simultaneously, reducing the body's capacity to manage each of these processes at the same time. The result is a compounding internal strain that does not plateau; it intensifies with each additional hour that food is withheld.
This is the metabolic reality that makes the earlier comparison to dogs and humans so important. In those species, some of these processes are slowed or adapted. In cats, they do not.
What happens inside your cat’s body isn’t random—it follows a clear biological pathway.
This visual model shows the difference between a healthy metabolic cycle and a dangerous breakdown process, so you can understand the risk at a glance.
🧠 Metabolic Pathway: Healthy vs Dangerous
See how feeding vs fasting affects your cat’s brain.
What is the arginine bottleneck in cats, and why is it dangerous?
Cats cannot produce sufficient arginine internally because they lack the intestinal enzyme needed to synthesize its precursor without dietary arginine; the urea cycle slows, and ammonia accumulates in the blood, creating a specific and serious neurological risk that is largely unique to cats among common domestic animals. This single biochemical gap sits at the center of why feline food deprivation carries consequences that have no real equivalent in dogs or humans.
Arginine is an essential substrate in the urea cycle, the biochemical process through which the liver converts toxic ammonia into urea for safe excretion. Most animals can synthesize some arginine internally through a pathway that requires an intestinal enzyme called pyrroline 5-carboxylate synthase. Cats lack this enzyme, making them almost entirely dependent on dietary arginine to maintain a functional urea cycle.
The consequences of this dependency were demonstrated in foundational research published in PubMed (Morris et al., 1979): near-adult cats given a single arginine-free meal after an overnight fast developed hyperammonemia, dangerous ammonia accumulation in the blood, and clinical symptoms of ammonia toxicity within two hours. One cat died within 4.5 hours. It is essential to note that this experiment used a specifically designed arginine-free diet, which is more extreme than natural fasting. Voluntary food refusal reduces arginine progressively rather than eliminating it instantly. Nevertheless, the research firmly establishes the principle: when arginine is unavailable, urea cycle function fails, and in cats, that failure can occur rapidly.
WikiVet, a peer-reviewed veterinary educational resource, reinforces this: cats are uniquely sensitive to dietary arginine deficiency, and hyperammonemia can develop within hours when arginine is absent from the diet. A case report published in PMC 2018 further demonstrated that arginine deficiency and hyperammonemia can develop in cats even without classical food deprivation in a cat with inflammatory bowel disease and chronic kidney disease that was receiving assisted nutrition but could not absorb amino acids adequately. This case highlights that the arginine bottleneck in cats is not exclusively a starvation risk but a fundamental feature of feline amino acid metabolism.
The practical implication for every cat owner is straightforward: when a cat stops eating, dietary arginine stops arriving, urea cycle efficiency begins to fall, and the body's ability to clear ammonia from the blood gradually diminishes. This is not a slow process, and it does not correct itself without food.
There’s a reason vets take appetite loss so seriously in cats—and it’s backed by research.
This insight reveals what actually happens in controlled studies when cats don’t get essential nutrients.
- Arginine is essential for removing ammonia from the body
- Without it, toxins can accumulate rapidly in the bloodstream
- This can directly affect brain function within hours
The Diet Switch That Backfired
James had been trying to do the right thing. His seven year old Ragdoll, Ptolemy, had put on weight over the winter, and after reading about calorie controlled feeding, James switched him from his usual wet food to a dry kibble with a lower fat content. Ptolemy sniffed it, walked away, and did not come back to the bowl.
James assumed it was pickiness Ptolemy had always been selective and figured he would come around once he got hungry enough. After about a day and a half, James noticed Ptolemy moving more slowly than usual and spending long stretches sitting in one spot rather than moving between his usual resting places.
At the veterinary clinic, the vet explained that Ptolemy's reluctance to eat the new food, combined with his existing weight, had created a situation where his liver was already beginning to work harder than it should. The vet also walked James through why cats cannot simply be transitioned to a drastically different food without a gradual changeover and why an overweight cat refusing food carries different risks than a lean one doing the same thing.
Ptolemy was transitioned back to his original wet food with a portion adjustment rather than a full food swap. Within a few days he was eating consistently again, and James began a much more gradual dietary transition plan under veterinary guidance.
Risk Stratification: Cats Most Vulnerable to Anorexia
Understanding that cats cannot safely skip meals establishes the general risk. But the picture becomes more nuanced and more practically useful when individual circumstances are factored in. Not every cat faces the same level of danger when food is withheld or refused, and the gap between a low-risk situation and a high-risk one can be significant.
The variables that determine how quickly a specific cat deteriorates include age, body condition, current health status, recent environmental changes, and the nutritional quality of the diet they were on before the fast began. Some of these factors accelerate the internal processes described in the previous section. Others reduce the metabolic buffer a cat has available before those processes reach clinically significant levels.
The Merck Veterinary Manual, revised in August 2023, identifies overconditioned cats as particularly vulnerable once anorexia begins. VCA Animal Hospitals similarly notes that the likelihood of serious complications is greater when a cat is overweight before the period of food refusal starts. But obesity is only one of several factors that can meaningfully shorten a cat's margin.
The following sections examine four distinct risk profiles: kittens, overweight or sick cats, cats under stress or on nutritionally poor diets, and cats at risk of fatty liver disease, and explain the specific mechanism behind each group's vulnerability. Understanding which category a cat falls into is one of the most useful tools an owner has for calibrating how urgently to respond.
Why are kittens more vulnerable if they stop eating?
Kittens face a significantly shorter window before food deprivation becomes dangerous because their energy reserves are extremely limited, while their metabolic demands are among the highest of any life stage. This combination means available fuel can be depleted within hours rather than the longer window a healthy adult cat might have. The risk profile for very young cats is categorically different from that of adults, and the timeline reflects this directly.
Cornell University College of Veterinary Medicine states that for a kitten younger than six weeks, food avoidance for just 12 hours can pose a lethal threat. That figure, half the already short 24-hour adult benchmark, reflects the compounding effect of two simultaneous physiological realities.
The first is the scale of energy demand. Kittens are growing rapidly across every system simultaneously; tissues, organs, bones, and immune function are all developing at once, each requiring a continuous and substantial energy supply. The second is the absence of meaningful reserves. An adult cat has fat stores and muscle mass that the body can convert, however inefficiently, into temporary fuel. A very young kitten has neither in any meaningful quantity. When food disappears, there is simply very little to draw on, and the deficit becomes critical far faster.
This is why kitten energy needs and the risk associated with food refusal must be understood as a separate category from adult cat risk. For kittens under six weeks, the response window is measured in single-digit hours rather than in days. For kittens between six weeks and several months, the margin is longer but still considerably shorter than in adults. Any kitten showing reduced food intake alongside behavioral changes warrants prompt veterinary attention without the wait-and-see approach that might be reasonable for a healthy adult cat in the very early stages of appetite change.
This quick checklist helps you identify whether your cat falls into a higher-risk category, so you can act earlier—not later.
Some cats are far more vulnerable to fasting-related complications than others.
⚠️ At-Risk Cat Checklist
Select all that apply to your cat:
Do overweight or sick cats decline faster without food?
Overweight cats face an elevated risk during food deprivation, not because excess weight provides a reserve, but because it accelerates liver stress. The larger the fat stores, the greater the volume of fatty acids mobilized to the liver when food is withheld, and the faster that organ becomes overwhelmed. For cats that are already ill, a compromised metabolic baseline means the body has less capacity to manage the additional strain that fasting creates.
This is one of the more counterintuitive aspects of feline health. Common sense might suggest that an overweight cat has more reserves to draw on and could therefore tolerate food deprivation for longer. In cats, the opposite is true. When food is withheld, the body signals fat stores to release fatty acids for conversion to energy. In an obese cat, this release is substantial and rapid. The liver receives more fatty acids than it can efficiently process or export, and fat begins accumulating within liver cells, a condition the veterinary community recognizes as feline hepatic lipidosis.
A large retrospective study of over 1.3 million cats seen at Banfield Pet Hospital practices across the USA between 2020 and 2023, Preventive Veterinary Medicine, 2024, found that nearly half of adult cats were classified as overweight, with obese rates highest in the mature cat age group. These are precisely the cats most frequently associated with hepatic lipidosis in the veterinary literature, not because their age alone increases risk, but because overweight mature cats combine the two primary vulnerability factors simultaneously.
For cats that are already unwell, the mechanism is different, but the outcome converges. Illness typically involves elevated metabolic demand from immune activity, potential reduction in liver or kidney function, and often some degree of pre-existing nutritional depletion. When food refusal compounds this, the body is managing multiple simultaneous strains with fewer resources than it would have in a healthy state. The decline under these conditions can move faster than it would in a cat starting from a position of full health.
How do stress and a poor diet increase the risk of not eating?
Stress and food refusal are a compounding combination in cats because the hormonal stress response actively accelerates the same catabolic processes that food deprivation triggers, meaning a stressed cat that stops eating is not simply dealing with two separate problems but with two forces pushing the same internal systems in the same direction simultaneously. A diet that was already nutritionally incomplete before the fast began reduces the buffer available even further.
The Merck Veterinary Manual 2023 specifically lists environmental stressors among the recognized triggers for feline anorexia: moving to a new home, the introduction of a new pet or person into the household, boarding, loss of a companion animal, and accidental confinement. These are not dramatic events in human terms, but for cats, animals strongly oriented around routine and territorial familiarity, they can suppress appetite meaningfully and for long enough to create real metabolic consequences.
The hormonal dimension of this matters beyond simply causing the cat to eat less. Stress hormones, particularly cortisol, promote protein breakdown and fat mobilization, the same internal processes that food deprivation drives independently. When both are active simultaneously, the rate at which the body depletes its amino acid reserves and generates metabolic waste is higher than either factor would produce alone.
A poor diet compounds this from the other direction. As established earlier in this article, cats require a continuous supply of specific essential amino acids that their bodies cannot conserve effectively. A cat that has been living on a nutritionally incomplete diet may already be deficient in some of these compounds before any period of food refusal begins. When fasting then reduces intake further, the starting buffer is smaller, and the threshold for clinically significant depletion is reached more quickly. The Merck Veterinary Manual notes that nutritional deficiencies, including cobalamin and arginine deficiency, are recognized contributors to hyperammonemia in cats, reinforcing that pre-existing dietary gaps can meaningfully shape how a cat responds to food deprivation.
Small mistakes are the biggest reason mild issues turn into emergencies.
This guide highlights the most common errors cat owners make—and what you should do instead.
Can skipping meals cause fatty liver disease in cats?
When a cat's food intake drops significantly, the liver becomes the primary site where the consequences accumulate. Fat mobilized from body stores arrives faster than the liver can process it, triglycerides build up within liver cells, and the resulting condition, feline hepatic lipidosis, can progress to serious liver dysfunction if food is not reintroduced. This is not a rare or extreme outcome; it is the most common acquired liver disease in cats, according to the Merck Veterinary Manual.
The development of hepatic lipidosis follows directly from the fat mobilization process that begins when energy from food is unavailable. The body signals adipose tissue to release fatty acids into the bloodstream. The liver receives these fatty acids and attempts to either convert them into usable energy through beta oxidation or package and export them as very low-density lipoproteins. In cats, particularly those who are overweight, the volume of incoming fatty acids can exceed the liver's capacity for both processes. The excess is stored as triglycerides within hepatocytes, the liver's primary functional cells, progressively impairing their ability to perform normal metabolic functions.
DVM360, drawing on veterinary proceedings data, notes that hepatic lipidosis accounts for approximately 50% of all liver disease diagnoses by biopsy in cats. A 2026 prospective study published in the Journal of Veterinary Internal Medicine, Oxford Academic, found that without aggressive intervention, mortality rates can exceed 90%, but the same body of evidence shows recovery rates of 90 to 95% with early, appropriate treatment. The gap between those two figures is the clearest argument for responding early rather than waiting.
An important nuance from the Ontario Veterinary College pet nutrition resource updated August 2025 is that hepatic lipidosis typically begins when food intake drops by 50 to 75% of normal, not necessarily to zero. A cat that is eating noticeably less but not refusing food entirely may still be on a trajectory toward liver stress if the reduced intake continues over several days. This distinction matters because it shifts the observation threshold: the question is not only whether a cat has stopped eating entirely, but whether intake has dropped meaningfully and for how long.
VCA Animal Hospitals notes that in more than 90% of cats with hepatic lipidosis, an underlying disease triggered the initial food refusal, reinforcing that the liver condition is often a signal that something else also needs to be identified and addressed alongside the nutritional support.
After the New Arrival
When Priya brought home a second cat a young tabby kitten she named Fig she had not anticipated how much the change would affect her existing cat, a nine year old Burmese named Cleo. Cleo had always been calm and easy going, so Priya assumed the adjustment would be smooth.
What she noticed instead, over the first few days after Fig arrived, was that Cleo was eating noticeably less. Not refusing food entirely, but leaving half the bowl untouched where she would usually finish everything. She was also spending most of her time in the bedroom which Priya initially interpreted as Cleo simply claiming her own space.
By day three, Priya mentioned the reduced eating to her vet during a routine call about Fig's vaccination schedule. The vet's response was more focused than she expected they asked specifically about Cleo's weight, her age, and how much her intake had dropped. When Priya described the pattern, the vet recommended bringing Cleo in given her age and the duration of reduced eating.
A check up confirmed that Cleo was in the early stages of stress related appetite suppression with some early metabolic indicators that warranted monitoring. The vet recommended separating feeding stations entirely and using a calming pheromone diffuser to ease the transition. Cleo's appetite returned to normal within a week, and the early identification meant there was nothing further to address beyond the environmental adjustment.
Clinical Timeline of Deterioration in Cats Without Food Intake
The previous sections established why cats cannot fast safely and which cats face the greatest risk of rapid decline. What remains and what many owners find most useful in practice is understanding how the internal changes described so far actually express themselves over time as observable symptoms.
This is where the biology becomes personal. A cat owner sitting at home watching their cat sit quietly near an empty bowl is not observing plasma arginine levels or urea cycle function. They are observing behavior, movement patterns, responsiveness, posture, and engagement. Understanding how those behavioral signals connect to the internal timeline, and at what point they cross from early-stage observation into something more urgent, is the practical core of this entire topic.
What the veterinary consensus makes consistently clear is that the progression from subtle to serious can happen faster than most owners expect and that the combination of symptoms alongside food refusal is more significant than either factor in isolation. The sections below trace that progression from the first quiet changes in the early hours, through the specific process of ammonia accumulation, to the point at which the situation requires prompt professional evaluation.
What happens in the first 12–24 hours if a cat doesn’t eat?
In the first 12 to 24 hours without food, the behavioral changes a cat shows, reduced activity, less engagement, a quieter and more withdrawn quality, are the observable expression of the internal metabolic shift that is already underway, not a separate phenomenon from it. Recognizing these early behavioral signals as metabolically connected rather than mood-related is one of the most useful shifts in perspective an owner can make.
The internal sequence driving these changes was established in detail in the earlier sections of this article. What matters here is understanding how that sequence looks from the outside. As glucose depletes and the body shifts to protein catabolism, energy availability changes. The cat's nervous system and muscles are receiving less efficiently produced fuel, and the behavioral result is a reduction in voluntary activity, less movement between rooms, less engagement with toys or people, and more time spent in one resting position.
Many owners describe this pattern in retrospect, after a veterinary visit has identified a developing issue. The early behavioral quietness seemed, in the moment, like a cat having a tired day. In hindsight, it was the first observable expression of a metabolic shift that had begun within hours of the last meal.
What makes the 12 to 24 hour window particularly important is that it represents the point at which these behavioral signals begin to be reliably visible, but before the situation has progressed to the more serious stages described in the sections that follow. Noticing them at this stage, in combination with confirmed food refusal, is the ideal moment for an owner to begin monitoring closely and to consider whether veterinary input is warranted based on the cat's individual risk profile.
A cat’s body doesn’t fail all at once — it deteriorates in predictable metabolic stages.
This visual timeline shows what’s happening inside your cat hour by hour, so you can recognize risk before it becomes an emergency.
⏱️ Cat Fasting Timeline
Tap each stage to see what’s happening inside your cat’s body.
• No major stress yet
• Mild hunger signals begin
👉 Action: Encourage normal feeding, no panic
• Liver begins processing fat load
• Appetite suppression may increase
👉 Action: Start active feeding strategies immediately
• Toxin buildup begins
• Symptoms may appear rapidly
👉 Action: Do NOT wait — seek veterinary care
How quickly does ammonia build up in cats without food?
Without a continuous dietary source of arginine, a cat's urea cycle becomes progressively less efficient and ammonia accumulates in the bloodstream, a process that begins during food deprivation and that, once it reaches neurologically significant levels, produces symptoms affecting brain function, including disorientation, unsteadiness, and altered responsiveness. The speed at which this accumulation becomes clinically meaningful depends on the individual cat's starting amino acid levels, body condition, and health status.
To understand this progression, it helps to recall the arginine bottleneck described earlier. The urea cycle converts toxic ammonia to urea for excretion, and this process requires arginine as a substrate. Cats cannot synthesize arginine internally in meaningful quantities, so when dietary intake stops, the available pool of arginine begins to fall. As it falls, urea cycle efficiency falls with it, and ammonia that would normally be cleared begins to accumulate.
Research from the Ontario Veterinary College, Verbrugghe and Bakovic, 2013, Nutrients, PMC confirms that plasma arginine concentrations can fall by more than 50% in cats experiencing food deprivation significant enough to cause hepatic lipidosis. A 2018 case report published in PMC documented a cat that developed acute neurological signs associated with severe hyperammonemia following persistent anorexia, demonstrating that the arginine deficiency timeline in real clinical cases can be meaningfully shorter than owners might assume.
Ammonia is neurotoxic. The brain and central nervous system are specifically sensitive to its accumulation, which is why the symptoms that emerge as ammonia builds are predominantly neurological in character: disorientation, unsteadiness, abnormal responses to stimulation, and, in advanced cases, altered consciousness. These are not symptoms that appear suddenly from nowhere. They are the endpoint of a progressive accumulation that began when food intake stopped, and arginine levels started to fall. Understanding this as a continuum rather than a sudden event helps explain why the early behavioral signals discussed in the previous section are worth taking seriously before they reach this stage.
Symptoms in cats don’t appear randomly — they progress in stages. This ladder helps you quickly identify how far the condition has advanced, so you can act at the right time—not too late.
🪜 Symptom Progression Ladder
Tap each stage to see how symptoms escalate.
• Mild lethargy
• Less playful behavior
👉 Action: Monitor closely and encourage feeding
• Avoiding food completely
• Irritability or unusual quietness
👉 Action: Start intervention immediately
• Weakness or unsteady walking
• Drooling or nausea
👉 Action: Urgent veterinary consultation needed
• Yellowing of eyes/gums (jaundice)
• Vomiting or refusal to move
👉 Action: Immediate emergency care required
When does not eating become life-threatening for a cat?
When a cat that is not eating begins to show physical or neurological signs like weakness, confusion, drooling, shaking, or trouble walking, the situation changes from one that needs close watching to one that needs immediate veterinary care. These signs mean the body’s internal problems have moved past the early stage where it can still cope. At this point, it is no longer just stress on the body but a serious crisis, and getting treatment quickly becomes much more important.
The Merck Veterinary Manual clearly explains the outlook for hepatic lipidosis, one of the main results of a cat not eating for a long time. With strong nutritional support and treatment, the condition usually improves within 14 to 21 days. If it does not improve, the cat does not survive. There is no long-term stable middle stage. Ongoing high bilirubin levels, low potassium, low albumin, and low blood pressure are warning signs. These show the condition has become very serious, and every extra hour without treatment becomes more critical.
Emergency signs that show the situation has become critical include extreme weakness or not being able to stand or walk normally, clear confusion, heavy drooling with no clear reason, muscle shaking, and a strong change in how the cat responds to its owner or surroundings. These signs show problems with the brain and nervous system. They happen because toxins like ammonia build up in the body during a severe metabolic crisis caused by long periods without food.
It is important to keep this in perspective. Most cats that miss one meal or eat less for a short time do not reach this stage. The progression described here shows what can happen if early warning signs are ignored or not treated, not what happens every time a cat skips a meal. The goal of explaining this process is not to cause fear, but to help owners clearly recognize the early signs if they appear.
DVM360, using data from veterinary reports, says that 90 to 95% of cats with hepatic lipidosis recover when they are given proper tube feeding and nutrition early enough. The Merck Veterinary Manual also confirms that cats who recover do not have lasting liver damage, scarring, or changes in liver structure. This shows the other side of the issue. When treatment starts early, the results are very good. A condition that causes more than 90% of cats to die without treatment has a 90 to 95% recovery rate with treatment.
The Quiet Decline Nobody Expected
Marcus had always described his cat Zephyr an eleven year old Maine Coon as the most low maintenance pet imaginable. Zephyr ate reliably, slept a lot, and was generally healthy. So when Zephyr began eating less over the course of about four days, Marcus initially read it as normal aging behavior. Older cats slow down, he reasoned. Appetites change.
What prompted him to call the vet was not a dramatic symptom it was the combination of things that had been quietly accumulating. Zephyr had not eaten more than a few bites in two days. He was moving very slowly when he did get up. And once, Marcus noticed him standing in the kitchen looking slightly disoriented, as though he had forgotten why he was there.
At the clinic, bloodwork showed that Zephyr's liver enzymes were elevated consistent with early hepatic lipidosis developing from several days of significantly reduced food intake. The vet began nutritional support through a feeding tube alongside treatment for an underlying thyroid issue that had likely been suppressing his appetite without producing obvious symptoms earlier.
Zephyr responded well to the intervention. After two and a half weeks of supported feeding and treatment for the underlying condition, his liver values normalized and he began eating independently again. Marcus reflected afterward that the individual signs had each seemed explainable on their own it was only when he looked at them together, and considered how many days they had been quietly building, that the picture became clear.
Conclusion: What Every Cat Owner Should Take Away From This
This topic could easily be presented in a way that scares cat owners into rushing to the veterinarian every time their cat skips a meal. But the evidence does not support that reaction, and it is not a helpful way for responsible owners to make practical, informed decisions.
What the evidence does support is something more specific and useful: cats have a metabolism that makes not eating more dangerous for them than for most other animals, and the time before it becomes medically serious is shorter than many owners expect. The risk factors for rapid decline include excess body weight, being middle-aged, living indoors with low activity levels, and having underlying but not yet visible health issues. Cats that are overweight, sedentary, and appear stable and healthy can actually be at higher risk of developing serious complications if they stop eating, even if they seem fine at first.
Understanding this is not a reason to panic. It is a reason to watch your cat closely and make informed decisions.
The Core Pattern Worth Remembering
Cats are obligate carnivores whose metabolism runs continuously on dietary protein. Unlike dogs or humans, they have no meaningful ability to reduce their rate of protein consumption during food scarcity. When food disappears, protein breakdown continues, ammonia is produced, and the urea cycle — which depends on dietary arginine that cats cannot synthesize internally — begins working with progressively less of what it needs.
The Cornell University College of Veterinary Medicine states directly that anorexia can have a severe impact on a mature cat's health if it persists for as little as 24 hours. For kittens under six weeks, that window shrinks to 12 hours. These figures come from standard institutional veterinary guidance and reflect how quickly feline physiology responds when nutrients are withdrawn.
The relationship between obesity and risk adds another layer. The 2022 Association for Pet Obesity Prevention survey found that 61% of cats in the United States are overweight or obese. A large retrospective study of over 1.3 million cats seen at Banfield Pet Hospital practices across the USA between 2020 and 2023 (Preventive Veterinary Medicine, 2024) found that nearly half of adult cats were classified as overweight, with obese rates highest in the mature cat age group. These are precisely the cats that face the greatest liver stress when food is withheld — not because their weight provides resilience, but because the volume of fat mobilized to the liver during fasting can exceed hepatic processing capacity.
Early Signs Are Subtle-That Is the Point
One of the most consistent themes across veterinary guidance on this topic is that the early signals of metabolic strain in a fasting cat are behavioral rather than dramatic. Reduced playfulness. More time spent resting. A quieter, less engaged quality that is genuinely easy to attribute to mood or a minor off day.
This is not because the internal changes are minor — it is because cats are naturally inclined to mask early discomfort. Noticing these subtle behavioral shifts and connecting them to appetite changes is genuinely useful. A cat that has not eaten for 12 to 18 hours and is also noticeably less active than usual is providing real information, even when nothing looks obviously wrong.
Keep track of when your cat last ate a full meal. Notice whether food intake has been slowly decreasing over several days. Pay attention to any recent changes in the environment, such as a new pet, a move, or a change in routine. Share this information with your veterinarian, as it provides directly useful context. These observations do not replace a professional exam, but they make the visit more effective and focused.
Some Cats Need a Shorter Response Window
The groups most likely to decline faster include kittens, overweight cats, cats that are already unwell, and cats that have recently experienced significant environmental stress. For any cat in these categories, the standard 24-hour mental benchmark for beginning to pay close attention may already be too long.
A kitten under six weeks that has not eaten for 12 hours, an obese adult cat that has refused food for a full day, or a recently ill cat showing both appetite loss and visible lethargy — these situations share a common feature: the metabolic margin is smaller than it would be in a healthy, lean adult cat, and the trajectory from early strain to serious complication can be shorter than the general timeline suggests.
This is not a reason to treat every missed meal as a crisis. It is a reason to factor individual circumstances into how quickly attention is applied. The same one-day food refusal looks meaningfully different in a lean, healthy five-year-old cat than it does in an overweight twelve-year-old cat with a history of digestive issues.
The Encouraging Part of This Picture
The reason early awareness matters so much in this topic is that the outcomes when intervention happens early are genuinely good. DVM360, drawing on veterinary proceedings data, notes that appropriate nutritional support results in recovery in 90 to 95% of affected cats with hepatic lipidosis when initiated at the right stage. The Merck Veterinary Manual confirms that cats who recover from hepatic lipidosis typically show no residual liver damage, no fibrosis, and no lasting structural changes.
The condition that is most dangerous without treatment is also one of the most treatable when caught early. Act as soon as you notice a problem instead of waiting to see if it resolves on its own. Early veterinary care greatly improves the chances of recovery and gives your cat the best possible outcome.
A Framework for Observation
Rather than a prescriptive checklist, consider this a set of questions worth asking when a cat's eating pattern changes:
- How long has it been since the cat last ate a full meal, and has intake been gradually declining over several days before that point?
- Is the cat showing any behavioral changes alongside the appetite shift — reduced movement, withdrawal, less responsiveness, or less engagement than usual?
- Does the cat fall into any of the higher-risk categories — very young, overweight, recently ill, or recently exposed to significant environmental change?
- Are there any visible physical signs accompanying the food refusal — weakness, unsteadiness, drooling, or unusual posture?
These are observational questions rather than diagnostic ones. Their purpose is to help a caring owner communicate clearly with a veterinarian and to support a timely, well-informed decision about whether and how urgently to seek professional input.
Closing Thought
Cats process food and energy differently from other animals. They are obligate carnivores, and their bodies do not handle food deprivation well. You do not need veterinary training to understand this. You need to pay attention to your cat’s eating habits and behavior.
Veterinary guidance from Cornell University College of Veterinary Medicine, the Merck Veterinary Manual, the Ontario Veterinary College, VCA Animal Hospitals, and research published through PubMed and PMC consistently supports the same message: notice changes early, monitor closely, and contact a veterinarian sooner rather than later. Do not panic. Do not assume the worst. Pay attention and act before the situation becomes serious.
Disclaimer: This article is for educational purposes only and is not a substitute for professional veterinary advice, diagnosis, or treatment. Always consult a licensed veterinarian if you have concerns about your cat’s health, diet, or behavior.
Frequently Asked Questions
Can a cat go without food overnight without any risk?
Most healthy adult cats can manage an overnight gap between their evening and morning meal without immediate metabolic concern. However, if the morning meal is also refused, that combined window begins moving into the range where closer observation becomes worthwhile.
Does drinking water help a cat that is not eating?
Water helps prevent dehydration but does not replace the amino acids and protein a cat's metabolism requires to function safely. A cat that is drinking but not eating is still at risk of the same internal metabolic changes that food deprivation triggers.
Can a cat recover fully after not eating for several days?
Most cats that receive appropriate veterinary care after a period of significant food deprivation recover without lasting organ damage. The Merck Veterinary Manual confirms that cats who recover from hepatic lipidosis typically show no residual liver damage or structural changes.
Is a cat that eats only a few bites still at risk?
A cat consistently eating only a fraction of its normal intake may still be on a trajectory toward liver stress even without complete food refusal. The Ontario Veterinary College notes that hepatic lipidosis can begin when intake drops by just 50 to 75% of normal over several days.
Do indoor cats face a different risk from not eating compared to outdoor cats?
Indoor cats may actually face a slightly elevated risk because they have fewer opportunities to supplement their intake independently and are more likely to be overweight — both factors that reduce their margin when food is refused. Outdoor cats may occasionally source food elsewhere, though this should never be relied upon as a safety buffer.
Resources and References
All data points, statistics, and expert guidance referenced throughout this article are drawn from the following verified, Tier-1 sources. Links were accurate at the time of publication.
Scientific and Peer-Reviewed Research
1. Peculiarities of One-Carbon Metabolism in the Strict Carnivorous Cat and the Role in Feline Hepatic Lipidosis Verbrugghe, A. and Bakovic, M. Nutrients — 2013 Cats cannot conserve arginine, taurine, and methionine; plasma levels of these amino acids fall by more than 50% during food deprivation. 🔗 Read on PMC
2. Ammonia Intoxication in the Near-Adult Cat as a Result of a Dietary Deficiency of Arginine Morris, J.G. et al. Science — 1979 Cats developed hyperammonemia within two hours of a single arginine-free meal; one cat died within 4.5 hours. 🔗 Read on PubMed
3. Experimental Induction of Hepatic Lipidosis in Cats Biourge, V. et al. American Journal of Veterinary Research — 1994 Hepatic lipidosis developed in 12 of 15 obese cats after 5 to 7 weeks of fasting; histologic changes confirmed in all 15. 🔗 Read on PubMed
4. Acquired Urea Cycle Amino Acid Deficiency and Hyperammonaemic Encephalopathy in a Cat PMC Case Report — 2018 Arginine deficiency and hyperammonemia developed without classic food deprivation, highlighting the broader fragility of feline urea cycle function. 🔗 Read on PMC
5. Hyperammonemia in Azotemic Cats Carvalho, L. et al. Journal of Feline Medicine and Surgery — 2021 Confirmed hyperammonemia across multiple feline disorders including arginine and cobalamin deficiency. 🔗 Read on PMC
6. From Anorexia to Obesity: The Role of Nutrition in Feline Diseases PMC / NIH — 2024 Cats cannot down-regulate their urea cycle or protein metabolism during starvation unlike dogs or humans. 🔗 Read on PMC
7. Preliminary Metabolic Characterization of Hepatic Lipidosis in Cats Journal of Veterinary Internal Medicine — 2026 Mortality exceeds 90% without intervention; epidemiologic patterns suggest higher incidence in middle-aged cats. 🔗 Read on Oxford Academic
8. Overweight and Obese Body Condition in 4.9 Million Dogs and 1.3 Million Cats Across the USA Preventive Veterinary Medicine — 2024 Nearly half of adult cats were overweight in a study of over 1.3 million cats seen at Banfield practices between 2020 and 2023. 🔗 Read on ScienceDirect
Professional and Institutional Veterinary Guidance
9. Feline Anorexia Cornell University College of Veterinary Medicine Anorexia can impact a mature cat's health in as little as 24 hours; for kittens under six weeks, 12 hours without food can be life-threatening. 🔗 Read at Cornell
10. Feline Hepatic Lipidosis Merck Veterinary Manual — Revised August 2023, Modified June 2025 The most common acquired feline liver disease; environmental stressors including moving and boarding are recognized anorexia triggers. 🔗 Read at Merck Veterinary Manual
11. Hepatic Lipidosis in Cats VCA Animal Hospitals Over 90% of cases involve an underlying disease; risk is greater in cats that were overweight before anorexia began. 🔗 Read at VCA Animal Hospitals
12. Obesity in Cats VCA Animal Hospitals 61% of U.S. cats are overweight or obese per the 2022 APOP survey; obese cats face significant hepatic lipidosis risk when food is withheld. 🔗 Read at VCA Animal Hospitals
13. Feline Hepatic Lipidosis Ontario Veterinary College Pet Nutrition — Updated August 2025 Hepatic lipidosis can begin when food intake drops by just 50 to 75% of normal; obese cats are most susceptible. 🔗 Read at Ontario Veterinary College
14. Hepatic Lipidosis DVM360 Veterinary Proceedings Accounts for approximately 50% of feline liver disease diagnoses; recovery rates reach 90 to 95% with early nutritional support. 🔗 Read at DVM360
15. Arginine Deficiency in Cats WikiVet — Veterinary Educational Resource Cats lack the enzyme to synthesize ornithine internally; an arginine-free diet can cause hyperammonemia and death within hours. 🔗 Read at WikiVet
Survey and Prevalence Data
16. 2022 U.S. Pet Obesity Prevalence Survey Association for Pet Obesity Prevention 61% of U.S. cats classified as overweight or obese by veterinary professionals — consistent since at least 2017. 🔗 Read at APOP
17. 2024 Pet Obesity and Nutrition Opinion Survey Association for Pet Obesity Prevention 33% of cat owners identified their pet as overweight in 2024; fewer than half were familiar with body condition scoring. 🔗 Read at APOP

Saloni Nagar is the founder and lead content creator of Bark & Meow Tales. As a dedicated cat parent and researcher, she transitioned from personal loss to pet health advocacy, focusing on early warning signs and preventive care. Saloni specializes in translating complex veterinary concepts into actionable guidance for pet parents. Her work is driven by a commitment to helping others interpret subtle feline health signals before they escalate, ensuring that every cat has a voice through informed, compassionate care.

